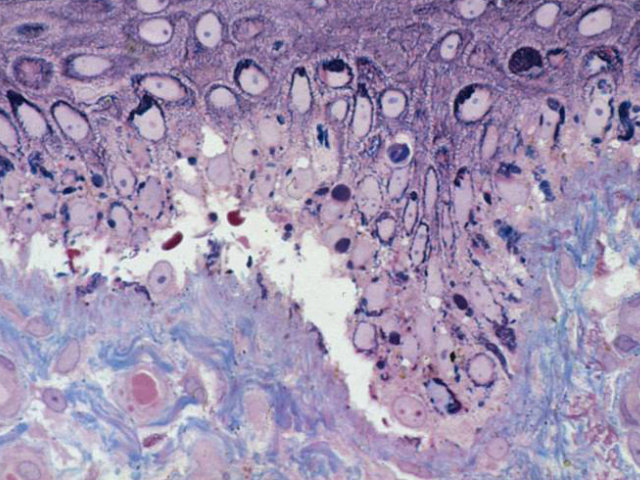
External skin and internal skin (mucous membranes) are affected, leading to blistering in the mouth and oesophagus (food pipe), and on the surface of the eyes. For a sufferer, this means that eating is always painful. Swallowing can be very difficult due to scarring of the oesophagus, necessitating balloon dilatation to allow food to pass. A small mouth opening (microstomia) and tongue scarring and contracture further make eating difficult. Many children and adults are fed via a gastronomy tube to allow adequate nutrition.
The fragile skin around the anal sphincter is similarly affected, leading to fissures, intense pain, and often constipation because of the pain associated with this everyday act. Laxatives and softeners are used on a daily basis in an attempt to combat this discomfort.
If the UV protective layer of the cornea is sheared off, the eye is vulnerable to UV light. The intense pain that this causes leads to a sufferer closing their eyes, rendering them temporarily blind till healing occurs.